Case Study: How Member Education and Engagement Guided Smarter Care Choices for a 2.6x ROI
How Valenz Bluebook Reduced Overall Plan Spend with Value-Based Healthcare Choices
Executive Summary
As the platform to simplify healthcare, Vālenz Health® offers solutions to support health plans in optimizing the cost, quality, and utilization of care for everyone.
A grocery chain in the Southwest partnered with Valenz for an innovative member engagement strategy that would guide smarter care choices to reduce overall plan spend.
Using a personalized communication strategy, Valenz Bluebook educated employees on in-network price variances, enabling them to make value-based healthcare decisions that delivered a program return on investment of 2.6:1 in the first year of implementation.
Sem Ipsum
Lorem ipsum dolor sit amet consectetur adipisicing elit. Ratione hic quaerat magnam accusantium sequi inventore non quod, maiores veniam recusandae maxime repudiandae impedit, obcaecati atque, iusto molestiae repellendus veritatis commodi illo ex ab! Maxime harum est ad suscipit sint delectus.
Challenge
A family-owned retail grocery chain in the Southwest with a large workforce of hourly employees sought creative ways to control growing medical spend without shifting too much of the financial burden to employees.
To complicate matters, a large percentage of employees only spoke Spanish and had little computer literacy, meaning health plan education had to be primarily conducted via mail.
Prior to the partnership with Valenz Bluebook, the client’s best line of defense against rising healthcare costs was to stress to employees the importance of choosing in-network providers.
After Valenz Bluebook demonstrated how in-network provider costs could vary as much as 600%, the client knew they needed a better strategy to encourage employees to make smarter, more cost-efficient healthcare choices.
Fusce a quam. Curabitur vestibulum aliquam leo. In dui magna, posuere eget, vestibulum et, tempor auctor, justo. Suspendisse eu ligula. Suspendisse non nisl sit amet velit hendrerit rutrum. Praesent egestas tristique nibh. Donec posuere vulputate arcu. Vestibulum turpis sem, aliquet eget, lobortis pellentesque, rutrum eu, nisl. Praesent metus tellus, elementum eu, semper a, adipiscing nec, purus. Sed libero.
I don't think anyone understood the drastic price variations that exist in your own network. Valenz Blubook introduced a new innovative approach to provide people with that information, because nobody was even thinking in those terms.
Member Benefits Representative
Long-term goal
Lorem ipsum dolor sit amet consectetur adipisicing elit. Ratione hic quaerat magnam accusantium sequi inventore non quod, maiores veniam recusandae maxime repudiandae impedit.
Solution
Using the Engagement Rewards feature, Valenz Bluebook worked with the client to create a direct mail campaign tailored to each employee demographic.
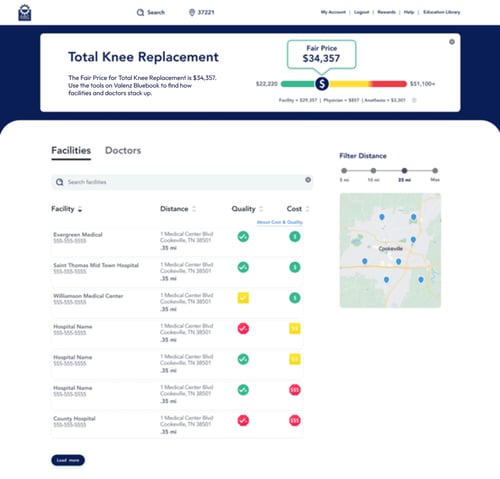
Employees received fun postcards and open enrollment packages demonstrating the simplicity of the Valenz Bluebook “green-yellow-red" methodology, which highlighted the high-value, low-cost care options available within the members’ network.
Every time an employee received a postcard or information about Valenz Bluebook via mail, program utilization increased as members began to shop for care. At the same time, detailed analytics allowed the client to view changes in healthcare shopping behavior as it occurred.
Valenz Bluebook integrated well with our insurance carrier, we loved implementation, and we achieved a positive ROI the very first year.
Member Benefits Representative
Results
As employees learned to use Valenz Bluebook to identify and schedule high-value care, more chose to receive care from “green”-labeled providers, resulting in direct savings for both members and the plan.
In the first year of implementation, the personalized strategy from Valenz Bluebook boosted average member program utilization rates to 10%, supporting cost savings in care choices that ultimately delivered a 2.6:1 return on investment for the client.
%20Case%20Study/colonoscopy-fair-price.png?width=500&height=188&name=colonoscopy-fair-price.png)
Conclusion: Capturing Savings Across Claim Complexity Comprehensive Payment Integrity Solutions
With a comprehensive, three-tiered approach to claim review, Valenz identified significant cost savings for this health plan payer, to a total tune of $43.4 million in allowed charges across a six-month period of claims with varying severity of impact.
While each tier of claims contributes measurably to overall financial incomes, the dramatic shift in provider attribution from the first to third level of severity suggests that a one-size-fits-all approach to payment integrity will underperform relative to differentiated strategies that incorporate both automated and manual claim review.
This payment integrity program demonstrates strong performance across all three levels, with clear evidence that a layered approach catches different types of billing problems — results that support investment in comprehensive, full-cycle payment integrity solutions that capture a wide variety and complexity of billed charge savings.
Lorem ipsum dolor sit amet consectetur adipisicing elit. Ratione hic quaerat magnam accusantium sequi inventore non quod, maiores veniam recusandae maxime repudiandae impedit, obcaecati atque, iusto molestiae repellendus veritatis commodi illo ex ab! Maxime harum est ad suscipit sint delectus.
Sarah Adams
Business Strategy Leader
Fusce a quam. Curabitur vestibulum aliquam leo. In dui magna, posuere eget, vestibulum et, tempor auctor, justo. Suspendisse eu ligula. Suspendisse non nisl sit amet velit hendrerit rutrum. Praesent egestas tristique nibh. Donec posuere vulputate arcu. Vestibulum turpis sem, aliquet eget, lobortis pellentesque, rutrum eu, nisl. Praesent metus tellus, elementum eu, semper a, adipiscing nec, purus. Sed libero.
%20Case%20Study/chart-movement-of-cases-from-high-cost-to-low-cost.png?width=1000&height=511&name=chart-movement-of-cases-from-high-cost-to-low-cost.png)